|
11/21/2023 0 Comments Quadruple aim healthcare 2021 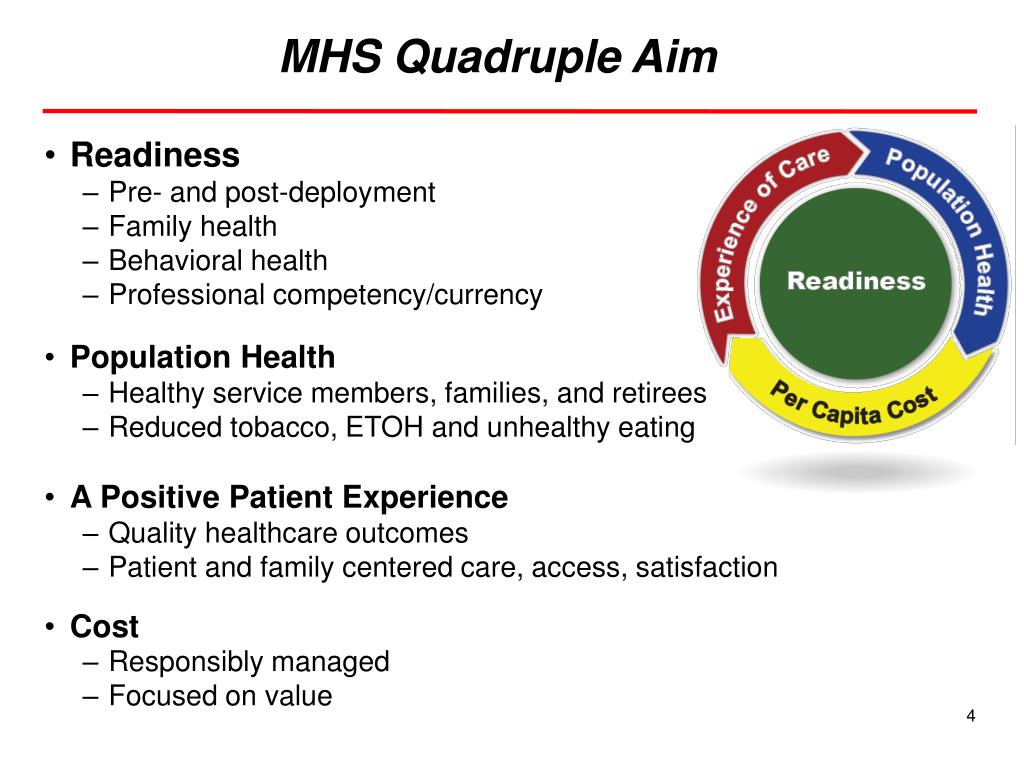
There is also another problem in the Netherlands, namely that many healthcare institutions and health insurers focus on budgets rather than the added value of treatment. However, there is still little scientific consensus on which outcomes are most relevant to patients and how they can best be measured. The concept of VBHC is actually an elaborated cost-effectiveness method from health economics. Porter indicates that a patient’s care pathway should be taken as the starting point, so that the added value of the various disciplines can be determined. 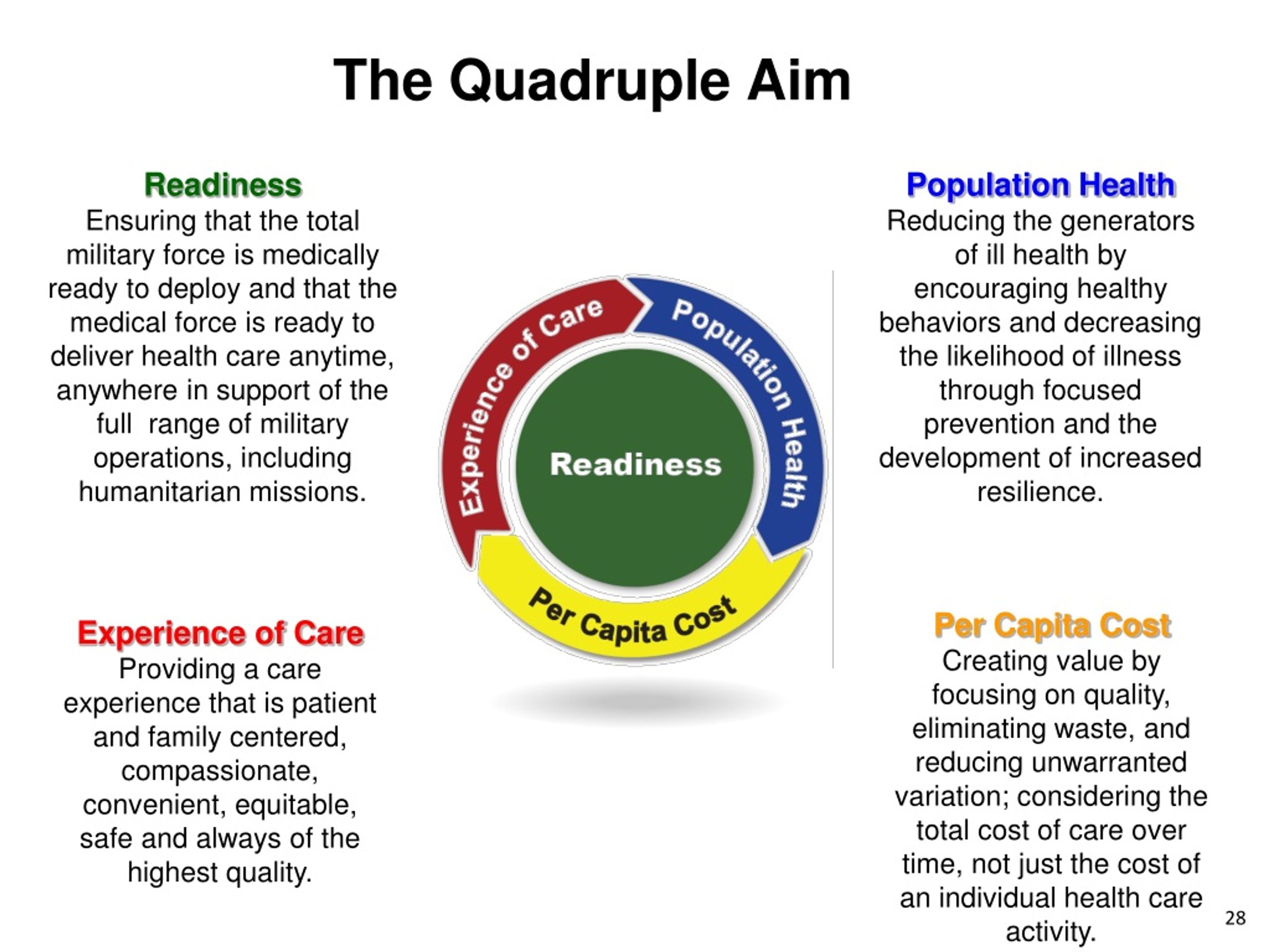
In the book ‘Redefining Health Care’, management expert Michael Porter describes VBHC as being about realising the best possible outcome for the patient at the lowest possible healthcare costs. Both VBHC and Triple Aim describe what value is, but both with a completely different focus. In the Netherlands, this is usually referred to as value-driven care. So no emphasis on just saving costs or excessive attention to stories of experience, but a balance that revolves around achieving the best care and health for the patient at the lowest possible cost. The care of the future is about creating multiple value, where economic, clinical and psychosocial values are in balance. In this blog I will make this clear by zooming in on the two concepts and then highlighting the three main differences. But is that right? Are the principles of both concepts the same? We can be brief about that: no. Both concepts originated in the United States and are often referred to in the same breath as value-driven care. Rising demand for and costs of care in the Netherlands. To find out how you can set your practice up for success with MIPS and Next Gen CCM, contact Richard Grosso at Scott Rice is CMO at Your Doctor In Touch.The 3 differences between Value Based Healthcare and Triple Aim you need to knowīoth Value-based healthcare (VBHC) and Triple Aim claim to be the solution for the Your Doctor In Touch promotes health and disease prevention through health caring. The Next Gen CCM innovation of pairing patient centricity with the QA creates synergy that increases patient satisfaction, improves patient outcomes, improves MIPS scores and promotes patient wellness. Patient satisfaction increases when they become engaged in their care.Ģ) Better outcomes for the Medicare patient population having multiple chronic conditions result from adherence to QA guidance and patient shared decision-making.ģ) Reduced Medicare costs result from increased patient wellness.Ĥ) Physician satisfaction increases and burnout decreases by having healthier patients, meeting MIPS requirements, and generating significant new revenue. Patient centricity is pivotal to advancing the QA in Next Gen CCM, and together these two value-added components of Next Gen CCM work together as follows:ġ) Patient experience of care is enhanced by focusing on what matters most to the patient. Therefore, YDIT has built a patient-centered culture by recruiting compassionate care managers who listen closely to patient priorities and provide them the most appropriate supportive CCM services. When patients believe health care professionals genuinely listen and act on what matters to them, they are more likely to be engaged in their care. From the beginning, Medicare CCM has required shared decision-making between practitioners and patients. Patient centricity is front and center in Next Gen CCM. YDIT has strategically embedded the QA to guide Next Gen CCM delivery. The four pillars are integrated to function in concert, so implementation of all four pillars is required for optimal effectiveness. The Quadruple Aim framework– enhanced patient experience of care, better health of populations, reduced health care costs and increased physician satisfaction – guides continuous improvement in health care. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
